Diabetes Subtypes
The Big Idea
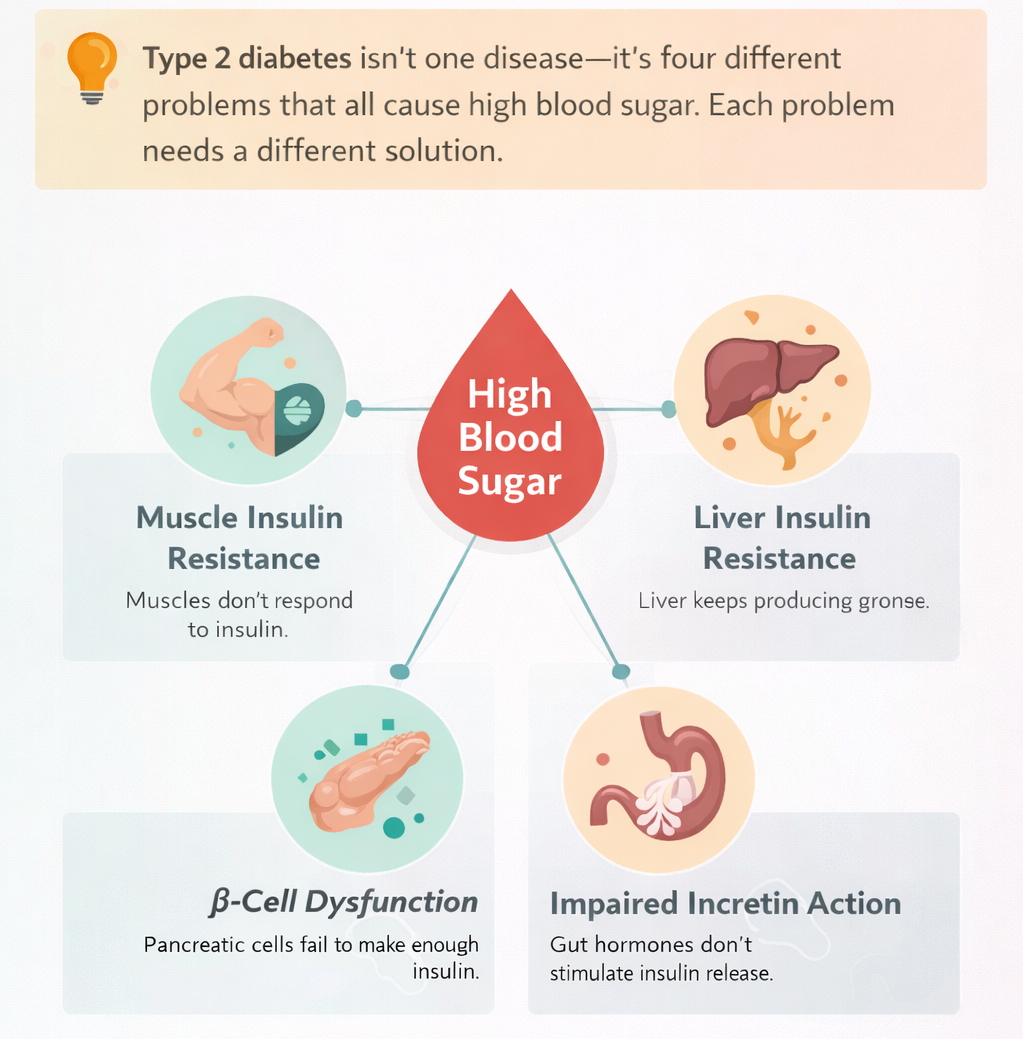
Type 2 diabetes isn’t one disease—it’s four different problems that all end up causing high blood sugar. Each problem needs a different solution. Think of it like a car that won’t start: the battery could be dead, the starter could be broken, you could be out of gas, or the fuel pump could be faulty. Same symptom, four different fixes.
Michael Snyder, PhD—Stanford’s W. Ascherman Professor of Genetics, co-led a study that reveals four key physiological subtypes underlying what we traditionally lump together as Type 2 diabetes (and prediabetes). These subtypes reflect distinct ways the body can mismanage blood sugar , and understanding them could pave the way for more tailored prevention and treatment strategies.
Based on continuous glucose monitoring (CGM) data and metabolic testing, the four identified subtypes are:
Diabetes Subtypes – Key CGM Patterns
| Subtype | Simple Explanation |
|---|---|
| 🔴 Liver IR | The liver continues releasing sugar into the blood even when the body does not need it, causing insulin resistance. |
| 🟠 Muscle IR | Muscles do not absorb sugar properly for energy, causing sugar to remain in the bloodstream and leading to insulin resistance. |
| 🟢 β-Cell Dysfunction | The pancreas does not produce enough insulin because the insulin-producing β-cells are damaged or reduced in number. |
| 🟣 Incretin Dysfunction | Hormones from the gut do not properly signal the pancreas to release insulin after eating, which affects blood sugar control. |
Traditional diagnosis of Type 2 diabetes relies heavily on blood sugar levels (e.g., fasting glucose or HbA1c), which don’t reveal these underlying mechanisms. This deeper classification into four subtypes:
- Helps explain why some patients respond differently to treatments (e.g. someone with β-cell dysfunction might benefit more from drugs that boost insulin production, whereas someone with insulin resistance might do better with insulin sensitizers).
- Opens the door for personalized treatment plans and targeted prevention, especially for those at risk.
- Leverages widely available CGM devices, making this personalized insight more accessible in everyday settings—not just specialized labs
The Four Problems & What to Eat
1. Muscle Insulin Resistance
— “Your muscles ignore the signal”
What’s happening: Insulin knocks on your muscle cells’ door, but they don’t answer. Sugar stays in your blood instead of going into muscles for energy.
Best foods: Lean proteins (salmon, chicken, eggs) + slow carbs (quinoa, lentils, beans). Add magnesium-rich foods (spinach, almonds, pumpkin seeds) and antioxidant-rich berries and citrus.
2. Liver Insulin Resistance
— “Your liver won’t stop making sugar”
What’s happening: Your liver is supposed to stop releasing sugar when insulin says “enough.” But your liver keeps pumping out sugar even when you don’t need it—especially at night.
Best foods: Omega-3 fish (salmon, sardines, mackerel), high-fiber foods (oats, barley, chia seeds), leafy greens and cruciferous vegetables (broccoli, kale). Black coffee and green tea are your friends.
3. β-Cell Dysfunction
— “Your insulin factory is struggling”
What’s happening: The beta cells in your pancreas can’t make enough insulin. When you eat, your blood sugar spikes fast and high because there isn’t enough insulin to handle it.
Best foods: Low-carb, low-glycemic choices to reduce insulin demand. Nuts and seeds (walnuts, chia, flaxseed), avocados, olive oil, and polyphenol-rich foods (blueberries, dark chocolate ≥70% cacao).
4. Impaired Incretin Action
— “Your gut hormones aren’t helping”
What’s happening: Normally when you eat, gut hormones (GLP-1, GIP) tell your pancreas “food’s coming, release more insulin!” These hormones aren’t working right, so your insulin response is delayed and weak.
Best foods: Fermented foods (yogurt, kefir, kimchi) to support gut health. High-fiber foods (apples, beans, lentils), resistant starch (cooled potatoes, green bananas), and protein at every meal.
🌟 Golden Rules for All Subtypes
- Avoid ultra-processed foods, sugary drinks, and refined carbs
- Eat whole foods with balanced macronutrients
- Physical activity (especially resistance training) helps all four subtypes
Summary Table
| Subtype | What’s Going Wrong |
|---|---|
| Muscle insulin resistance | Insulin not effectively helping muscles take up glucose |
| Hepatic insulin resistance | Insulin failing to suppress glucose production by the liver |
| β-cell dysfunction | Pancreas not producing enough insulin |
| Impaired incretin action | Gut hormones (incretins) failing to support insulin secretion |